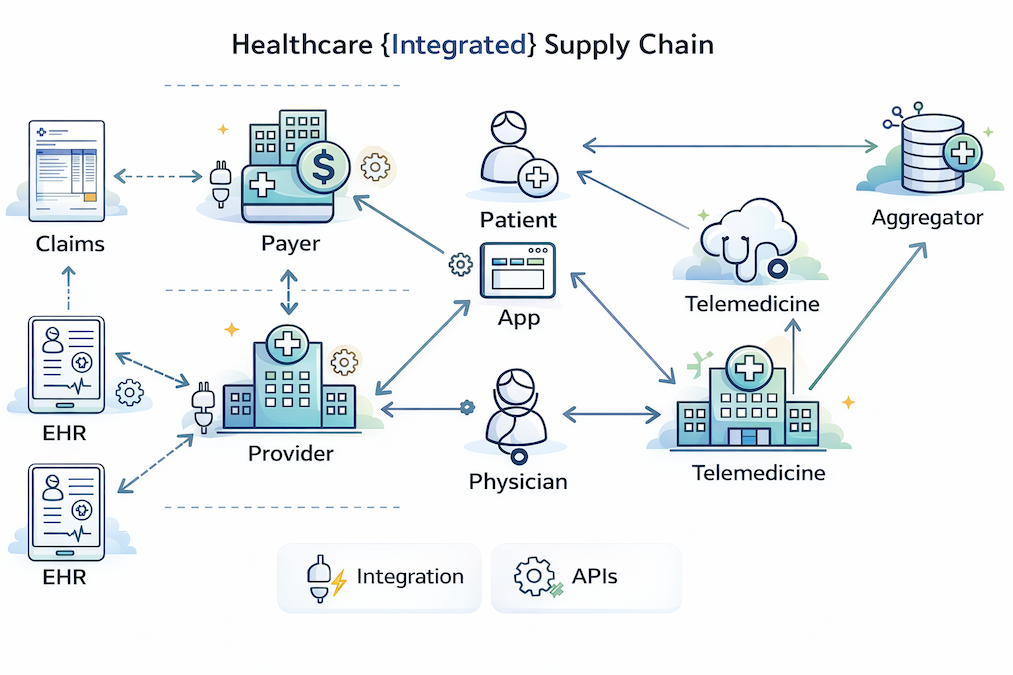
Healthcare organizations today operate in an environment where data is one of their most valuable assets, yet much of that data remains locked inside disconnected systems. Hospitals, clinics, and provider networks spend millions each year attempting to integrate Electronic Medical Records (EMRs), billing systems, patient portals, telehealth platforms, and analytics tools.
One of the most effective solutions to this challenge is FHIR (Fast Healthcare Interoperability Resources) — a modern interoperability standard that allows healthcare systems to exchange data seamlessly using standardized APIs.
While FHIR is often discussed from a technical perspective, its financial impact on healthcare organizations is equally transformative. For hospitals and large provider networks, adopting a FHIR-based interoperability strategy can dramatically reduce IT integration costs, increase operational efficiency, and create new revenue opportunities.
Understanding FHIR in Healthcare Infrastructure
FHIR is a modern interoperability standard developed by Health Level Seven (HL7) that enables secure and structured healthcare data exchange between systems.
Unlike older healthcare messaging standards that require expensive custom integrations, FHIR uses modern web technologies such as RESTful APIs, JSON, and OAuth authentication, making it easier and less expensive to implement.
The Financial Impact of FHIR Adoption
1. Reduced Integration Costs
Traditional healthcare integrations require:
- Custom HL7 interfaces
- Expensive middleware
- Vendor-specific interfaces
- Months of development time
Each integration can cost anywhere from $20,000 to $250,000 depending on complexity.
FHIR dramatically reduces these costs by enabling:
- Standardized APIs
- Reusable integration frameworks
- Faster implementation cycles
Organizations adopting FHIR can reduce integration costs by 40–70% compared to legacy HL7 interface development.
2. Lower IT Maintenance Expenses
Healthcare organizations often maintain hundreds of legacy interfaces between systems. Each of these requires:
- Continuous monitoring
- Software updates
- Interface engine maintenance
- Vendor support contracts
By moving to a FHIR-based architecture, hospitals can reduce the number of custom interfaces and shift toward a centralized interoperability layer.
This leads to:
- Lower infrastructure costs
- Fewer integration failures
- Reduced engineering workload
For large health systems, this can result in millions in annual IT operational savings.
3. Faster Implementation of New Technologies
Healthcare innovation is accelerating rapidly. Organizations frequently need to implement:
- Telehealth platforms
- Remote patient monitoring
- AI diagnostic tools
- Patient engagement apps
- Population health analytics
Without interoperability standards, each new platform requires expensive custom integration.
FHIR allows hospitals to deploy new technologies much faster, often reducing integration timelines from months to weeks.
This enables providers to adopt new technologies without disrupting existing systems.
4. Improved Revenue Cycle Efficiency
FHIR enables real-time data exchange between clinical and billing systems, which can significantly improve revenue cycle performance.
Benefits include:
- Faster insurance verification
- Automated prior authorization workflows
- Improved claims accuracy
- Reduced billing errors
These improvements directly impact revenue by reducing claim denials and accelerating reimbursements.
For large healthcare organizations, even a 1–2% improvement in revenue cycle performance can represent millions of dollars annually.
5. Compliance with Federal Interoperability Regulations
The FHIR standard is central to regulatory requirements such as the CMS interoperability rules and patient access APIs.
Hospitals that proactively implement FHIR are better positioned to comply with federal mandates including:
- Patient access APIs
- Provider data exchange requirements
- Prior authorization interoperability
Early adoption reduces the risk of expensive compliance retrofits and ensures healthcare organizations remain aligned with evolving federal policy.
6. Enhanced Data Analytics and Population Health
FHIR enables healthcare organizations to aggregate structured data across multiple systems.
This makes it significantly easier to implement:
- Population health programs
- Predictive analytics
- AI-driven clinical insights
- Value-based care reporting
By unlocking data across the enterprise, healthcare organizations gain the ability to optimize care delivery while controlling operational costs.
Strategic Advantage for Hospitals and Provider Networks
Healthcare is transitioning toward a fully interoperable digital ecosystem, where providers, patients, and payers exchange information in real time.
Organizations that adopt FHIR today gain several long-term advantages:
- Lower integration costs
- Faster digital innovation
- Improved operational efficiency
- Better regulatory compliance
- Increased ability to leverage healthcare data
Hospitals that delay interoperability adoption risk becoming trapped in expensive legacy infrastructure that slows innovation and increases operational costs.
The Future of Healthcare Interoperability
FHIR is rapidly becoming the foundation of modern healthcare data exchange.
Major healthcare technology companies, government agencies, and EMR vendors are investing heavily in FHIR-based architectures.
For hospitals and provider networks, the question is no longer whether to adopt FHIR, but how quickly they can transition to an interoperable architecture that reduces costs and improves efficiency.
Healthcare organizations that prioritize interoperability today will be best positioned to deliver better care, lower operational costs, and sustainable financial performance in the digital health era.