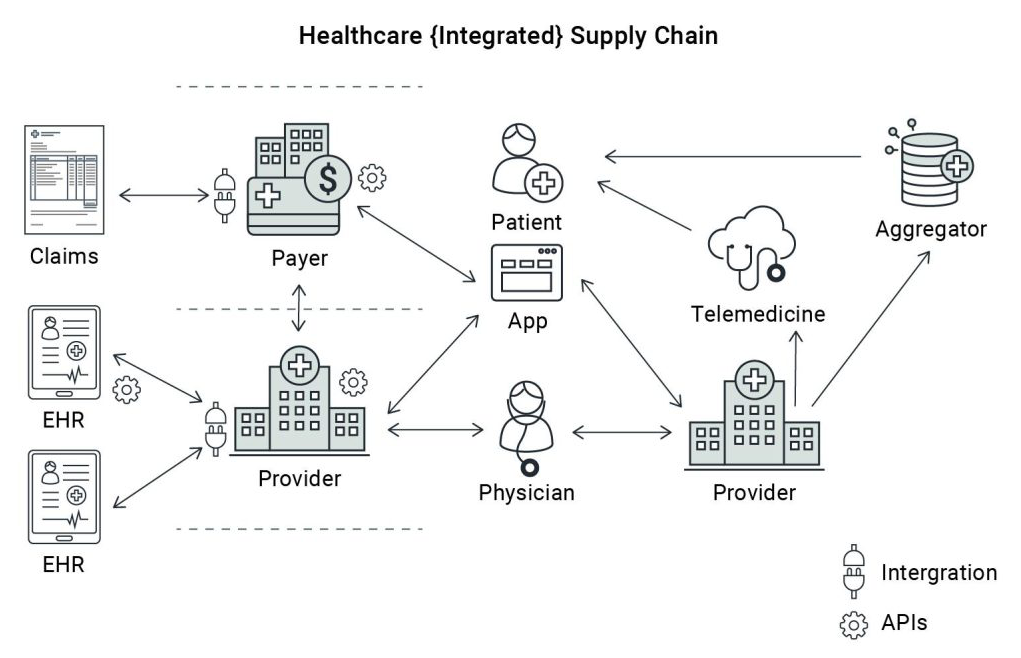
Healthcare interoperability has long been a buzzword in industry corridors — but today, it’s evolving into a strategic imperative. At the center of this transformation is FHIR (Fast Healthcare Interoperability Resources), a modern API-centric standard that’s reshaping how we share, access, and use health data. While larger health systems have begun tapping into its potential, small private practices stand on the brink of a similar revolution — one that promises better care coordination, reduced administrative burden, and new pathways to value-based care.
In this post, we’ll unpack why FHIR matters for small practices, what opportunities it unlocks, and practical steps you can take now — before your competitors do.
Why FHIR Isn’t Just for Big Health Systems Anymore
FHIR may have started as the data standard of choice for large hospitals and enterprise EHR vendors — but its simplicity, flexibility, and modern API design make it an ideal fit for smaller, nimble practices.
Here’s why:
- Modern Data Sharing Without Proprietary Barriers
FHIR uses RESTful APIs, JSON and XML formats — the same building blocks used in mainstream web and mobile applications. That makes integration with third-party tools smoother than legacy HL7 interfaces. - Patient-Centered Data Access
Through standards like SMART on FHIR and patient-facing APIs, practices can empower patients with seamless access to their own records — boosting engagement and satisfaction. - Foundation for Innovation
FHIR isn’t just about exchanging notes — it’s the backbone for telehealth apps, decision support tools, NLP summarization services, quality reporting engines, and more.
What FHIR Can Enable for Small Practices
Small private practices often struggle with administrative complexity and data fragmentation — two areas where FHIR delivers tangible gains:
🚀 1. Better Clinical Decision Support
When data from labs, imaging centers, and hospitals flows into your workflow in real time, clinicians can make faster, more accurate decisions. FHIR makes this data accessible and usable within the tools your team already uses.
📊 2. Smarter Quality Measurement
Quality programs like MIPS and value-based contracts rely on timely, actionable data. FHIR’s structured resources make quality reporting both easier and more accurate — enabling practices to optimize performance and revenue.
🤝 3. Smoother Care Coordination
Patients often see multiple providers, yet their records are scattered. FHIR acts as a lingua franca, enabling true interoperability across ambulatory care, specialists, labs, and payers.
📱 4. Patient Engagement and Digital Tools
Mobile apps and patient portals that leverage FHIR give patients modern experiences — from viewing records to sharing data with family caregivers.
The Immediate Actions You Must Take — Starting Today
Harnessing FHIR isn’t a distant dream — it’s something you can begin building toward right now. Here’s how:
1. Audit Your Current Data Landscape
Before you innovate, you need clarity.
- What systems are you using (EHR, labs, imaging, billing)?
- Can they already expose FHIR APIs?
- Where do data silos exist?
This audit will inform your integration strategy.
2. Evaluate EHR and Vendor FHIR Support
Not all FHIR implementations are equal.
- Ask your EHR vendor: Which FHIR version do you support (R4, STU3)?
- What resources are currently available (Patient, Observation, Condition, MedicationRequests)?
- Do they support OAuth2 / SMART on FHIR for secure third-party access?
You might find that your systems already support many FHIR endpoints — it’s just a matter of activating them.
3. Prioritize Use Cases With Immediate ROI
You don’t need to solve every interoperability challenge at once. Start with high-impact use cases:
✅ Automated quality reporting
✅ Lab order/results integration
✅ Referral coordination and care transitions
✅ Patient access via apps and portals
These deliver measurable ROI early in your FHIR journey.
4. Invest in Developer Resources
FHIR thrives on APIs — and APIs require developers.
- Hire or partner with developers experienced in RESTful APIs and healthcare data
- Consider low-code/no-code integration platforms that support FHIR (e.g., integration engines, iPaaS solutions)
- Work with third-party innovators who already use FHIR to build value-added services
5. Build a Governance Framework
Data exchange must be secure and compliant.
- Establish policies for API access and data sharing
- Define roles for who can provision apps and third-party integrations
- Ensure compliance with HIPAA and patient consent requirements
Sound governance protects your patients and your practice.
The Strategic Advantage Ahead
At its core, FHIR levels the playing field. Small practices that embrace it now will enjoy:
- Fewer administrative headaches
- Better clinical outcomes through connected care
- Stronger patient engagement and loyalty
- Operational readiness for future payment models
Conversely, those who delay risk being locked into costly integrations and falling behind in value-based care innovations.
Conclusion: The Future Is API-Driven — Don’t Get Left Behind
FHIR isn’t a distant industry buzzword — it’s the operational backbone of healthcare’s next decade. For small private practices, embracing FHIR isn’t optional; it’s strategic.
To thrive, start with data discovery, build use cases that deliver immediate value, and purposefully adopt APIs that enhance workflows and patient experience. The future of healthcare is interoperable — and the practices that harness FHIR today will lead it tomorrow.